- Ankle Arthritis
- Anterior Ankle Impingement and Bone Spurs
- Posterior Ankle Impingement and Os Trigonum
- Ankle Fracture
- Ankle Instability
- Ankle Syndesmosis Injury
- Osteochondral Lesions of the Talus (OLT)
- Tibialis Posterior Tendon Dysfunction
- Plantar Fasciitis
- Hindfoot Arthritis
- Lesser Toe Deformity
- Achilles Tendon Disorders
- Achilles Tendon Rupture
- Peroneal Tendon Disorders
- Calf Strain
- Ganglions
Ankle Arthritis
Arthritis occurs when smooth cartilage lining the joint becomes worn leading to increased friction as the bones rub together. This leads to pain in the affected joint which tends to become more pronounced as the cartilage wear progresses. Arthritis in the ankle, in contrast to that of the hip or knee, often occurs secondarily as a result of previous injury. There may be a series of minor injuries or history of repeated ankle sprains with microtrauma to the articular cartilage accumulated over a number of years.
Symptoms and Progression
The symptoms of ankle arthritis include pain around the ankle joint, particularly during walking or exercise. Arthritis can lead to swelling, and significant stiffness in the affected joint. In particularly severe instances, ankle arthritis can lead to deformity of the joint, which can make walking difficult.
Arthritis sufferers commonly live with the symptoms for a number of years before seeking treatment. Ankle arthritis will tend to slowly progress with intermittent painful exacerbations and remission of symptoms.
Diagnosis
A careful clinical history and examination is usually sufficient to suggest ankle arthritis however a standing X-ray of the ankle will demonstrate joint space narrowing, malalignment, small bone cysts and other areas of eburnated or worn bone. X-ray is the most useful investigation for arthritis since most cross-sectional imaging (CT and MRI) can only be performed non-weight bearing. X-rays can also help determine whether there are small bone spurs called 'osteophytes' arising from the margin of the joint which can give rise to soft tissue entrapment in the joint or 'impingement'.
Non-Operative Treatment
Non-operative treatment for ankle arthritis aims to reduce the pain arising from the joint while maintaining a degree of mobility. In order to reduce the contact pressure across the degenerate ankle one of the single most important measures is weight-loss and activity modification.
Activities that repetitively load the ankle joint such as running should be avoided and instead range of motion exercise to overcome stiffness commenced. Cycling and swimming in this respect are ideal. A formal course of physiotherapy may also be beneficial. It may be appropriate for work-place adaptations or restricted duties to be considered, particularly during painful exacerbations of arthritis.
Specialised footwear can help with pain, either by providing stability to the ankle during walking, or by cushioning the impact on the joint. A stiff-soled shoe incorporating a rocker sole can be very useful in reducing the arc of motion demanded from the ankle during walking.
Pain-killers and anti-inflammatory medication can also reduce symptoms, if there is no other medical objection to the patient taking them.
Steroids given directly into the joint can give temporary relief but repeated administration should be avoided. When used in combination with a local anaesthetic agent, usually under image-guidance (ultrasound or X-ray) injections can help confirm the ankle as the source of pain when adjacent hindfoot or midfoot joints are also arthritic.
Surgery
'Key-hole' or arthroscopic surgery to the ankle joint can often be very useful when the majority of the joint is in good condition with a good range of remaining movement. Arthroscopy is often employed to burr away prominent bone spurs arising from the margin of the joint and causing soft tissue entrapment or 'impingement' in the ankle. In addition it is an excellent method of visualising the articular cartilage in the joint and assessing suitability for future operative intervention.
On occasion, by removing bone spurs in the ankle and increasing its range of motion, the improved movement on the degenerate cartilage can increase pain so its use has to be judicious.
In severe cases of joint malalignment a boney cut or 'osteotomy' is used to correct joint alignment but this tends to be reserved for early cases of arthritis where the condition of the articular cartilage is well preserved.
The gold standard treatment of end-stage ankle arthritis remains ankle fusion or 'arthrodesis'. This treatment has been in existence since the 1960s and remains the most reliable way of eliminating the pain caused by arthritis by preventing the joint moving. Patients tolerate a fusion very well and it is often difficult to tell that a someone has undergone an ankle fusion by the way they walk, provided there is still a degree of mobility in the remaining hindfoot and midfoot joints.
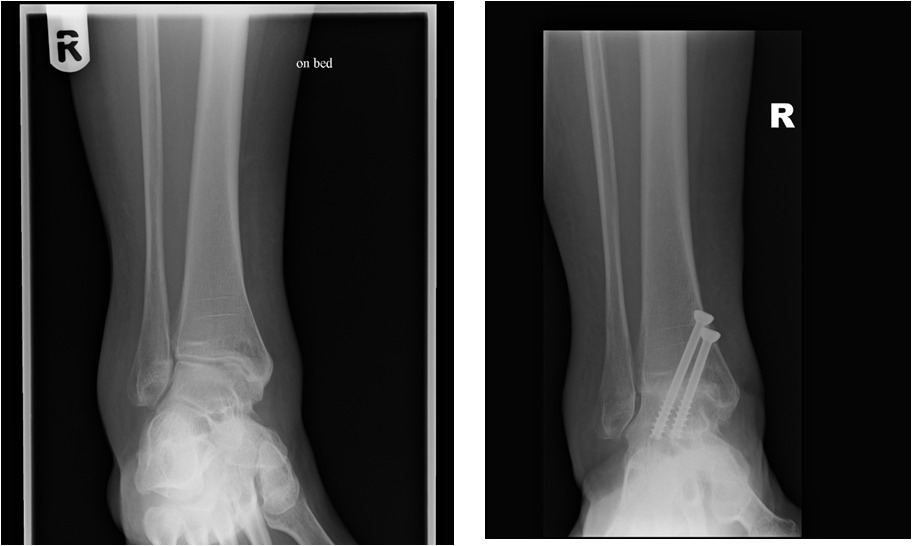
Ankle fusion (known as Ankle Arthrodesis) involves the surgical removal of the remaining cartilage around the arthritic joint, usually utilising a key-hole technique followed by the ankle being fixed into a functional position with either screws alone or sometimes with a metal plate. The individual bones making up the ankle then slowly fuse as one bone thereby removing the ankle as the source of pain.
Ankle arthroplasty is a rapidly advancing science and recent medical literature reports a high level of success with ankle joint replacement. A patient's individual suitability for ankle replacement needs detailed pre-operative counselling.





