- Ankle Arthritis
- Anterior Ankle Impingement and Bone Spurs
- Posterior Ankle Impingement and Os Trigonum
- Ankle Fracture
- Ankle Instability
- Ankle Syndesmosis Injury
- Osteochondral Lesions of the Talus (OLT)
- Tibialis Posterior Tendon Dysfunction
- Plantar Fasciitis
- Hindfoot Arthritis
- Lesser Toe Deformity
- Achilles Tendon Disorders
- Achilles Tendon Rupture
- Peroneal Tendon Disorders
- Calf Strain
- Ganglions
Tibialis Posterior Tendon Dysfunction
The Tibialis Posterior tendon arises from a muscle attached to the back of the tibia (shin bone) and runs down behind the ankle on the inside of the leg. It is one of the larger tendons of the region, and is important in the support of the the foot's structure, maintaining its natural arch and permitting forward propulsion during walking.
Tibialis Posterior tendon dysfunction is a condition where the tendon becomes damaged due to inflammation leading to a number of symptoms and changes within the foot.
This condition is usually caused by overuse of the tendon which tends to occur as a result of extended periods of walking, running, climbing stairs, any type of repeated exercise without adequate recovery, and undue load on the tendon due to obesity.
Symptoms and Progression
The symptoms of Tibialis Posterior tendon dysfunction vary depending on the severity of the condition.
In the early stages the patient will feel activity-related pain along the inside of the foot and ankle where the tendon is located. This may be accompanied by discolouration and swelling.
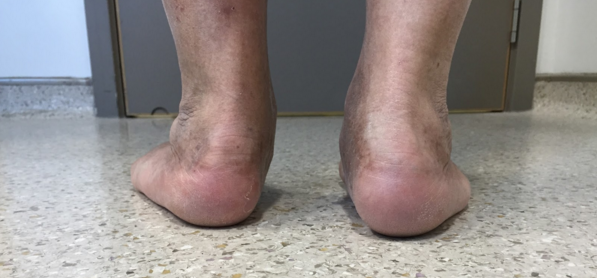
As the damage to the tendon increases the arch of the foot will begin to fall and flatten, causing the toes and the hindfoot to turn outward.
As this continues, pain can also arise on the outside of the hindfoot around the bottom of the ankle. In particularly advanced cases, the degradation of the Tibialis Posterior tendon with consequent changes to the structure of the foot can lead to arthritis of the foot and ankle.
Diagnosis
Following a careful clinical examination, standing X-rays of the foot and an Ultrasound scan of the tendon will confirm the diagnosis. Occasionally an MRI may be performed.
Non-Operative Treatment
If treated early, the condition can often be treated without the need for surgery.
In acute tendonitis a specialised walking cast can provide foot and ankle immobilisation which prevents the tendon from working in order to give it time to rest and recover. This is a temporary measure, usually employed over a period of six weeks to settle acute inflammation after which time the walking boot can be replaced by an insole worn in the shoe. This is occasionally not desired or suitable, so custom-made orthotics can be used as an alternative.
Physiotherapy to strengthen the Tibialis Posterior tendon is often beneficial, particularly in early stages of the disease. You may be given a bungee-cord or 'Theraband' which is an excellent method of exercising the tendon against resistance as well as specific exercises to stretch-out the much larger calf muscle (gastrocnemius) that acts as a deforming force on the hindfoot.
There are many other additional self-help measures such as the administration of simple anti-inflammatory medication (NSAIDS such as ibuprofen taken orally as tablets or topical anti-inflammatory gels). One of the most effective measures is weight loss to reduce the load on the diseased tendon and wearing suitable lace-up supportive foot-wear.
Surgery
In cases of failed non-operative treatment or if the condition is already too advanced, a Tibialis Posterior Reconstruction is often beneficial.
This procedure may involve simple removal of portions of the diseased part of the tendon (debridement and repair). However when the Tibialis Posterior tendon is severely degenerate another sacrificable tendon located behind the Tibialis Posterior tendon in the midfoot called the Flexor Digitorum Longus (FDL) involved in flexing the lesser toes Is used as a donor tendon to reconstruct the Tibialis Posterior tendon.
This is a relatively simple procedure, requiring only a single incision on inside of the ankle, and does not affect the patient's ability to bend their toes to any great degree.
The FDL tendon transfer is almost always combined with a Calcaneal Osteotomy which involves making an incision on the outside of the calcaneum (heel bone) in order to undertake a heel shift which re-directs the pull of the Achilles tendon to the midline, restoring hindfoot alignment and supporting the tendon reconstruction. The osteotomy is secured internally with a screw which remains in situ and does not usually require removal.
In severe cases of Tibialis Posterior tendon dysfunction there may be symptoms and signs of midfoot, hindfoot or even ankle arthritis. The presence of arthritis and fixed deformity in the ankle and hindfoot may require different operations such as a fusion or 'arthrodesis'.





