- Ankle Arthritis
- Anterior Ankle Impingement and Bone Spurs
- Posterior Ankle Impingement and Os Trigonum
- Ankle Fracture
- Ankle Instability
- Ankle Syndesmosis Injury
- Osteochondral Lesions of the Talus (OLT)
- Tibialis Posterior Tendon Dysfunction
- Plantar Fasciitis
- Hindfoot Arthritis
- Lesser Toe Deformity
- Achilles Tendon Disorders
- Achilles Tendon Rupture
- Peroneal Tendon Disorders
- Calf Strain
- Ganglions
Osteochondral Lesions of the Talus (OLT)
What is it?
In contrast to ankle arthritis, where there is diffuse, chronic degeneration of the friction-reducing articular cartilage, osteochondral lesions are focal single injured areas of cartilage in an otherwise normal, well-functioning ankle.
What is it caused by?
OLT present in active, sporty individuals who may describe a past severe ankle sprain which caused a shear-injury of the cartilage. Occasionally they present insidiously as part of an underlying bone blood-supply problem although this is rare.
Symptoms
Articular cartilage does not have a nerve or blood supply. You can therefore happily “wear-it-down” until a point when the underlying bone which does have a nerve and blood supply, becomes irritated. This is similar to the way in which a dental cavity may present itself and infact the cold-weather pain associated with OLT has been compared with tooth-ache.
An unstable OLT may have a flap which catches and clicks in the ankle and there may be ankle swelling and restricted walking ability. Approximately 1/20 acute ankle sprains cause the development of an OLT so any worrying symptom persisting after 6-8 weeks of an ankle sprain warrants thorough clinical evaluation.
Diagnosis
Unless very large and involving bone, an OLT will not be visible on X-ray although X-rays might well be used to initially exclude an ankle fracture or an alignment or stability problem in your ankle.
MRI is the most sensitive initial investigation for OLT. Occasionally a CT scan or a CT arthrogram may be used to evaluate the OLT stability or when a bone cyst is associated with an OLT.
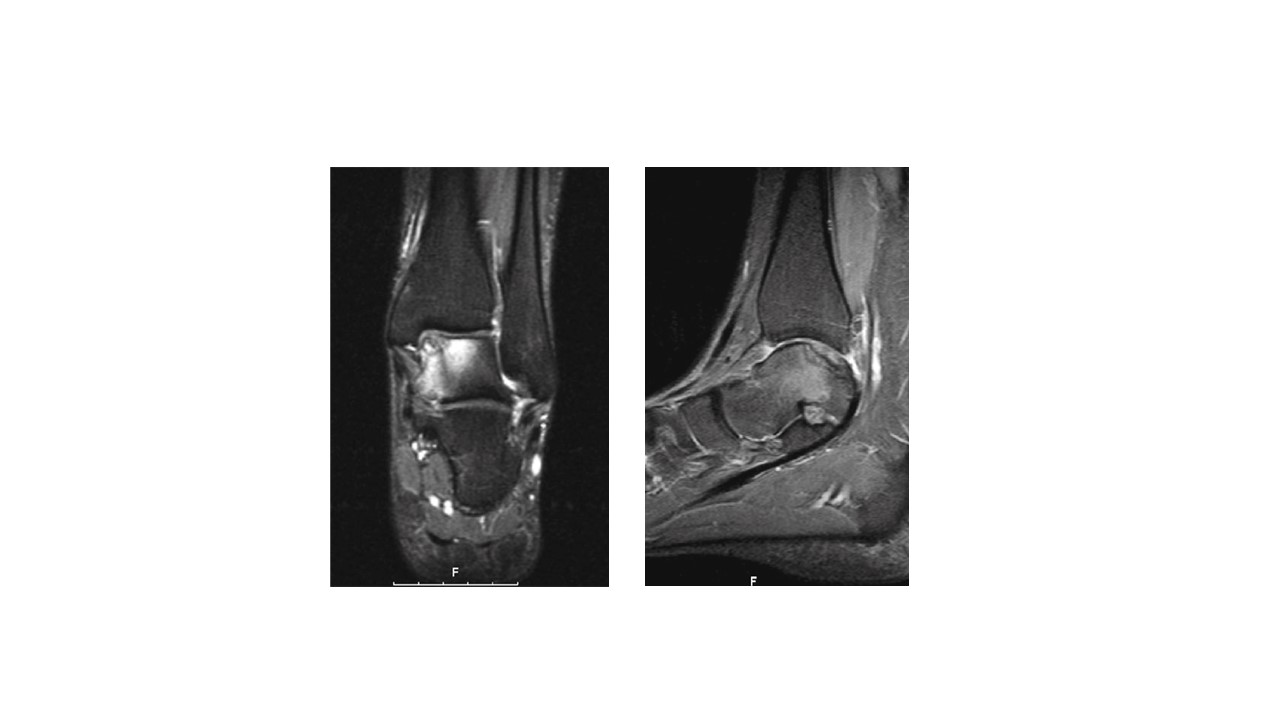 MRI scan-fluid-weighted sequence (above) showing a large medial talar dome osteochondral lesion (OLT) with surrounding bone-marrow oedema. A CT arthrogram was performed (below) to determine the dimension of the underlying bone cyst and its communication with the ankle joint (there almost always is a communication through a one-way flap valve mechanism)
MRI scan-fluid-weighted sequence (above) showing a large medial talar dome osteochondral lesion (OLT) with surrounding bone-marrow oedema. A CT arthrogram was performed (below) to determine the dimension of the underlying bone cyst and its communication with the ankle joint (there almost always is a communication through a one-way flap valve mechanism)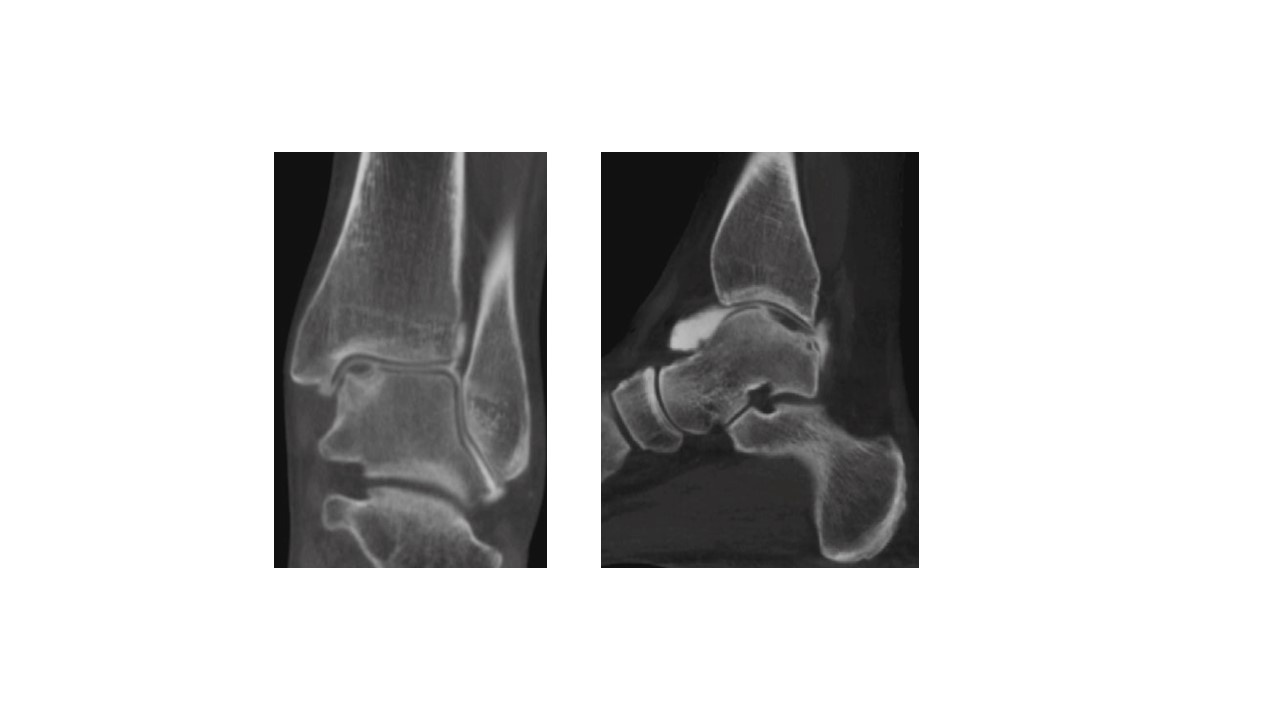
Non-Surgical Treatment
Treatment of these cartilage lesions is most often surgical. A short period of non-weight-bearing, avoidance of sport and bracing has most often been tried due to the co-existing ankle instability that accompanies most OLTs. Steroid injections into the ankle joint should as a rule not be given, since they reduce the chances of healing the OLT. Where ankle stability is co-existent, physiotherapy can be enormously helpful, both pre- and post-operatively.
Surgical
Arthroscopic assessment and treatment is the standard management of OLT. This allows a thorough evaluation of the dimensions of the lesion and permits simultaneous treatment.
Arthroscopic microfracture involves removal of any unstable, non-viable flap of cartilage and surrounding inflammatory tissue and puncture of the hard bone in the base of the OLT. This causes the bone to bleed, releasing growth factors carried in platelets which will invoke a healing response.
The cartilage generated as a result of microfracture is not pure hyaline cartilage with the properties your un-injured cartilage has. Rather, it is a mix of fibrocartilage and hyaline cartilage which in the majority of cases (80-90%) is enough to adequately treat the pain and seal over the defect.
Larger areas of cartilage loss, or patients who have not improved following initial microfracture surgery may benefit from cartilage regenerative techniques. This surgery is usually more invasive, requiring larger skin incisions and occasionally bone cuts around the ankle to permit adequate access to the injured area. The surgery involves taking either a sample of patient’s centrifuged blood, rich in platelets and injecting them under a special biological matrix which holds the cells in place while they generate cartilage- a procedure called “Autologous Matrix-Induced Chondrogenesis” (AMIC). Or whole plugs of cartilage can be transplanted from a non-weight-bearing are of the knee to fill in the void- a procedure called “Osteochondral Autograft Transplant” (OATS).
For more significant, deep cartilage lesions involving underlying bone cysts it is often necessary to take a small bone graft from the patient to implant under the cartilage cell matrix. Further options include partial prosthetic replacements of the talus which can work well in lower demand patients with sedentary lifestyles.





