- Ankle Arthritis
- Anterior Ankle Impingement and Bone Spurs
- Posterior Ankle Impingement and Os Trigonum
- Ankle Fracture
- Ankle Instability
- Ankle Syndesmosis Injury
- Osteochondral Lesions of the Talus (OLT)
- Tibialis Posterior Tendon Dysfunction
- Plantar Fasciitis
- Hindfoot Arthritis
- Lesser Toe Deformity
- Achilles Tendon Disorders
- Achilles Tendon Rupture
- Peroneal Tendon Disorders
- Calf Strain
- Ganglions
Plantar Fasciitis
Plantar Fasciitis is a condition which is characterised by pain in the heel and the bottom of the foot. This is caused by inflammation of the plantar fascia, the thick lining that runs along the sole of the foot. Anatomically and functionally, the plantar fascia acts as a tie-bar to the longitudinal arch of the foot, preventing its collapse on weight-bearing and helping the foot become a rigid lever for forward propulsion during walking.
The causes of this inflammation are not always clear, but overuse and constant stress on the bottom of the foot are thought to contribute. Prolonged periods of walking or running, particularly on hard surfaces or in hard-soled footwear can sometimes lead to the condition. Obesity is the highest modifiable risk factor for plantar fasciitis. Increased body weight means a higher degree of pressure on the bottom of the foot.
The co-existence of other foot and ankle conditions causing higher pressure on the heel due to mechanical imbalance can also make plantar fasciitis worse. General inflexibility of the calf and hamstring muscles, as well as reduced mobility in the ankle joint can also lead to a greater degree of stress being placed on the heel.
Symptoms and Progression
Heel pain is the primary symptom of this condition, though pain may also be felt in the arch of the foot. In particular, sufferers of Plantar Fasciitis tend to experience the most pain after periods of inactivity, for instance when first standing up as they get out of bed.
Little happens to progress the condition over time, and many people live with the pain and inflammation for years before seeking treatment. It is possible for the condition to resolve itself, but without any sort of action taken to encourage it, this can take over 18 months.
Diagnosis
Although the symptoms and signs of plantar fasciitis are classic, if there are any atypical features in the presentation then imaging is important. A weight-bearing X-ray of the foot may highlight a calcaneal insufficiency or stress fracture. The presence of 'heel spurs' on an X-ray is often seen in association with plantar fasciitis and it does NOT mean the solution to the disease is their surgical removal.
An ultrasound scan of the plantar fascia is very helpful in confirming the condition by measuring the plantar fascial thickness as well as examining for the presence of tears.
Cross-sectional imaging techniques such as MRI and Nerve conduction studies are rarely needed to diagnose plantar fasciitis but may occasionally be required if there is doubt about the diagnosis and a suspicion that there may be another cause of the heel pain.
Non-Operative Treatment
Plantar Fasciitis is generally treated with a range of non-operative interventions, and rarely requires surgery. Around 90% of Plantar Fasciitis cases will improve within six months of treatment.
Patience and determination is important in the treatment of plantar fasciitis. One of the most important self-help measures is weight loss as undoubtedly reducing the load on the heel is beneficial. It is important to avoid bare-foot walking and to wear appropriate lace-up shoes. A programme of acupunture can be very helpful.
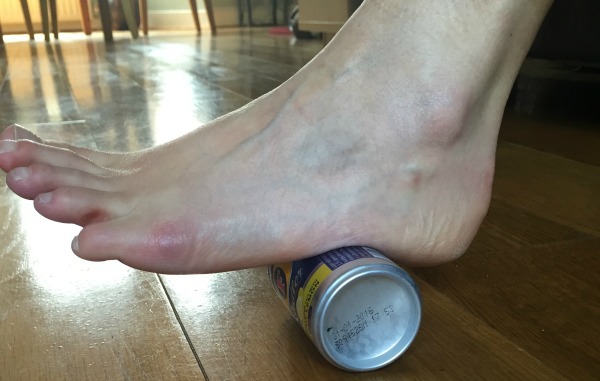
A programme of physiotherapy can have a significant impact on the condition, utilising stretches and exercises to improve the mechanical function of the foot. Eccentric gastrocnemius stretches are one of the most beneficial modes of physiotherapy in reducing the pull of the calf muscle on an inflamed plantar fascia, since the two are effectively in continuity through the heel bone. A night-splint can be very helpful in a patient with a tight calf muscle who is particularly affected by morning symptoms.

Heel pads and insoles will help to absorb the impact of walking, allowing the inflammation of the fascia more opportunity to recover. Occasionally with an acute exacerbation of the condition, complete immobilisation of the leg and off-loading in a plaster cast is needed.
Extracorporeal shockwave therapy (ESWT), a technique which delivers mild shockwaves to the plantar fascia can also help reduce symptoms of Plantar Fasciitis and induce healing of the inflamed tissue.
The use of nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen also have a high degree of success when it comes to treating this condition.
Corticosteroid injections are a rarer and less predictable form of treatment, but are sometimes used if other forms of intervention have failed to significantly improve a patient's condition. They should always be administered under ultrasound guidance to avoid inadvertent injection of other important structures in the foot.
Surgery
Surgery is rarely needed for this condition. Many referrals for 'heel spurs' build an expectation that simple spur removal will improve the condition. These spurs are almost always in the non-weight bearing area of the heel and occur as a consequence of chronic inflammation of the plantar fascia. They are not the cause.
Proximal Medial Gastrocnemius Recession (PMGR):
Provided at least 6 months of good quality physiotherapy, weight loss and trialing of all the aforementioned non-operative measures have elapsed with no discernable benefit PMGR can be considered. Not all patients with plantar fasciitis are appropriate for this surgery. Evidence of gastrocnemius (calf muscle) tightness must be detected on clinical examination before this technique is considered.
Plantar fasciotomy:
Simple division of the plantar fascia is not a recommended treatment. There are plenty of alternative treatments with lower risk to the function of the foot. The potential complications of this technique are far more disabling and difficult to treat.





